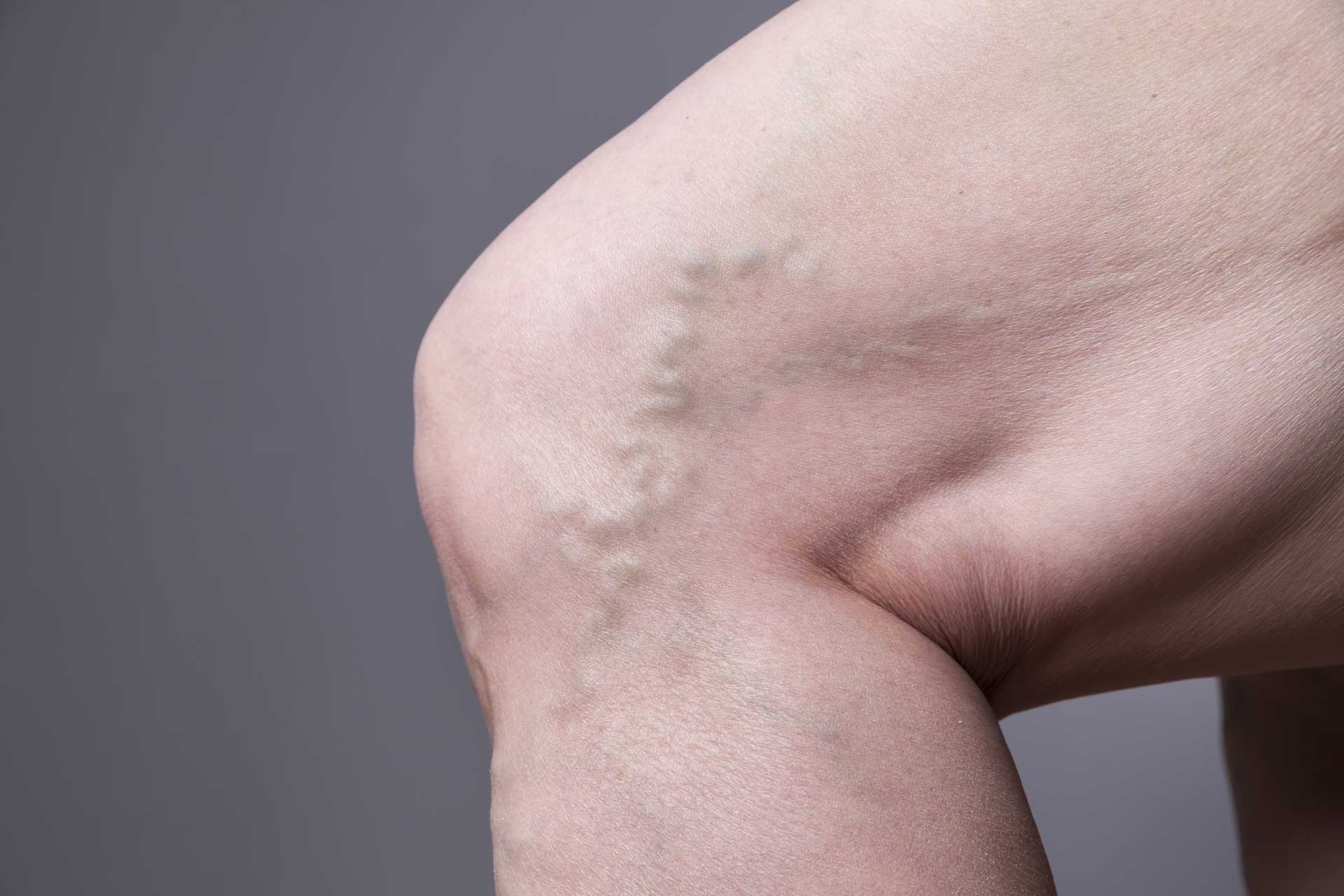
VARICOSE VEINS
VARICOSE VEINS TREATMENTS
Radiofrequency Ablation (RFA), also known as endovenous thermal ablation, is a modern, minimally invasive procedure for treating varicose veins. It’s a popular alternative to traditional surgical vein stripping.
How It Works: A small catheter is inserted into the abnormal vein, typically the great saphenous vein (GSV), using ultrasound guidance. Radiofrequency energy is delivered through the catheter, generating heat that causes the vein to collapse and seal shut. Once the vein is closed, blood is naturally redirected to healthier veins nearby. The treated vein is then absorbed by the body over time.
Key Features:
- Minimally invasive with no large incisions.
- No general anesthesia required, only local anesthesia is used to numb the area.
- The procedure is quick, often completed in about an hour.
Patient Experience: Patients can typically walk immediately after the procedure and can return to normal activities within a day. A mild sensation of warmth or pressure may be felt during the procedure. Post-procedure bruising and soreness are common but usually mild.
Vein Stripping & Ligation
Vein stripping and ligation is a traditional surgical procedure for treating severe cases of varicose veins. It is a more invasive option than modern, minimally invasive treatments like RFA or VenaSeal.
- How It Works: The procedure involves making small incisions in the groin and, in some cases, at the ankle or calf. The surgeon then ties off (ligates) the top of the damaged vein to stop blood flow. A thin, flexible wire is then threaded through the vein, and the entire vein is removed (stripped) through one of the incisions.
- Key Features:
- This is a surgical procedure that requires incisions.
- General or regional anesthesia is typically used.
- The entire diseased vein is physically removed from the body.
- Patient Experience: While effective, vein stripping has a longer recovery time compared to minimally invasive procedures. Patients may experience significant bruising, swelling, and discomfort for a few weeks after the surgery. Full recovery can take 2 to 4 weeks.
Varithena is a non-thermal, non-tumescent procedure that uses an injectable microfoam to treat incompetent great saphenous veins (GSV) and other related veins.
- How It Works: A trained physician uses ultrasound guidance to inject the Varithena foam into the targeted vein. The foam fills the vein, causing it to collapse and seal shut. The body then naturally absorbs the treated vein.
- Key Features:
- No incisions or stitches are required, as the procedure is performed through a single needle puncture.
- The microfoam displaces blood and treats the vein walls, causing the diseased vein to collapse.
- The procedure is quick, often lasting less than an hour.
- Patient Experience: Patients typically experience minimal discomfort and can resume most normal activities on the same day. Compression stockings are usually required for about two weeks after the procedure.
VenaSeal is a non-thermal, non-sclerosant procedure that uses a specially formulated medical adhesive to permanently close varicose veins.
- How It Works: Using ultrasound guidance, a small catheter is inserted into the diseased vein. A small amount of medical adhesive is then delivered into the vein, and light external pressure is applied to seal the vein walls together. Blood is immediately rerouted to healthy veins.
- Key Features:
- This procedure uses a medical-grade glue and does not rely on heat (thermal energy), which eliminates the need for multiple anesthetic injections.
- Typically, only one needle stick is needed for the entire procedure.
- There is no need for tumescent anesthesia or sedation.
- Patient Experience: Patients report minimal to no pain during the procedure and can often return to their normal activities immediately. A major advantage of VenaSeal is that compression stockings are typically not required after the procedure.